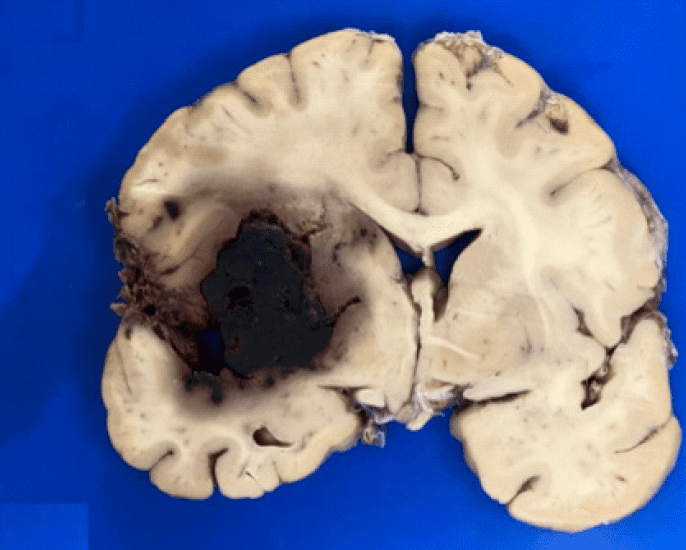
Preprint: Autopsies reveal Covid-19 brain damage
SARS-CoV-2 related coagulation disorders are the main cause of the brain tissue damage. Most of the brain damage was related to thrombosis.
We investigated the neuroinvasive potential of SARS-CoV-2, searching for morphological and microbiological features of viral involvement of the central nervous system (CNS) in individuals who died of COVID-19 related respiratory failure during the first pandemic wave (February–April 2020).
SARS-CoV-2 RNA was retrieved from the olfactory bulbs and tracts and from the brain tissue in 1 out of 11 patients only, while most of the brain damage was related to thrombosis.
During the second and the third pandemic waves (November 2020–April 2021), a further 22 brain autopsies were performed. SARS-CoV-2 RNA was searched in all cases and transmission electron microscopy (TEM) was also added to detect the viral particles on positive specimens
The data here shown are consistent with data presently published and features indicate that:
- SARS-CoV-2 can directly infect the central nervous system, even if it is not clear which is the direct type of brain tissue damage.
- Morphological features indicate that SARS-CoV-2 related coagulation disorders are the main cause of the brain tissue damage. The immediate use of anticoagulant therapy in critical patients reduced thromboembolic complications.
- Bacterial superinfection can be the cause of acute leptomeningitis during SARS-CoV-2 infection.
- Brain damage can be present even in absence of specific neurological symptoms. Therefore, it is possible that brain involvement could be an underestimated feature in SARS-CoV-2 infected patients.
- Astrogliosis, microglial activation and chronic inflammation could play a role for the development of chronic neurological disorders.
Preprint: COVID-19 and the Brain: The Neuropathological Italian Experience on 33 Adult Autopsies
13% of hospitalized Covid-19 patients developed neurological conditions including encephalopathy