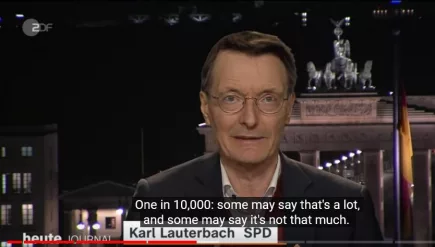Category: Symptoms
Texas: H5N1 bird flu confirmed in a human
Texas has confirmed its first case of H5N1 avian flu in a human today. More...
UK NHS healthcare workers launch group litigation against government for Covid-19 injuries received at work
UK NHS workers are preparing to take legal action against the British government for failing to protect them during the Covid-19 pandemic. More...
Censored by TikTok: Gastroenterologist reveals damage to human microbiome by vaccines
“Their bifidobacteria dropped to like zero – from like a million to like zero – there was a persistence in the damage, not only 90 days but 6-9 months later. More...
Germany: One in 10,000 vaccinated for Covid are severely injured by the jab
Germany’s Health Minister, Karl Lauterbach, has stated in an interview that around one person in ten thousand is severely injured as a result of a Covid-19 vaccination. More...
Cambodia: 12 more infected with H5N1 bird flu following death of an 11yr old girl *5 updates*
Cambodia’s health department is reporting that 12 more people have been infected with H5N1 Avian flu following the death of a 11yr old girl from the virus yesterday. More...
Long Covid fatigue caused by an Arginine deficiency
The mechanism that leads to chronic fatigue in Long Covid patients has been discovered, according to new Italian research. More...
US: Nearly 19 million adults may have long COVID
A new US population-based survey suggests that nearly 19 million adults in the US may have long COVID. More...
Israeli head of biological research: I was wrong three times when I was vaccinated
Prof Shmuel C. Shapira MD MPH, head of the Israel Institute for Biological Research for 8 years, on being vaccinated for Covid three times. More...
Elon Musk: I had major side effects from my second booster shot
Elon Musk: “I had major side effects from my second booster shot. More...
WHO: Rapid Risk Assessment for XBB.1.5 published
The World Health Organisation has issued a rapid risk assessment for the Omicron XBB.1.5 variant (aka Kraken), which we are republishing below. More...