Category: Infection
Anthony Fauci canvasses a black neighbourhood to convince them to take the Covid-19 vaccine
It doesn’t go as planned.
Anthony Fauci strolls around an unknown Black neighborhood trying to convince residents that they should get vaccinated, claiming that it will protect their families from Covid-19 transmission if they have it. More...
Texas: H5N1 bird flu confirmed in a human
Texas has confirmed its first case of H5N1 avian flu in a human today. More...
Highly Pathogenic Avian Influenza in Cattle in Texas, Kansas, New Mexico, Idaho and Michigan *14 updates*
The U.S. Government has announced that highly pathogenic avian influenza (HPAI) has been found in cattle in Texas and Kansas. More...
UK NHS healthcare workers launch group litigation against government for Covid-19 injuries received at work
UK NHS workers are preparing to take legal action against the British government for failing to protect them during the Covid-19 pandemic. More...
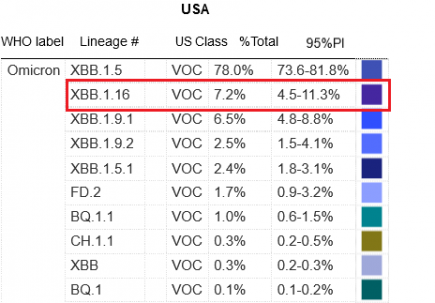
XBB.1.16 is the second most common variant in the US
XBB.1.16 has debuted on the CDC Covid variant list today in SECOND PLACE. More...
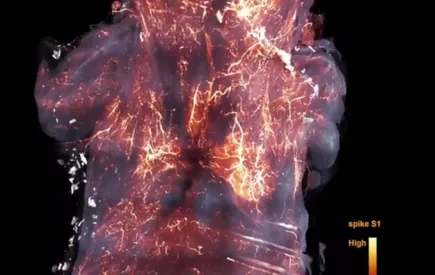
SARS-CoV-2 spike protein accumulates in the brain
A new study out today offers sobering evidence of the extent of infection and damage caused by the SARS-CoV-2 spike protein in the human body. More...
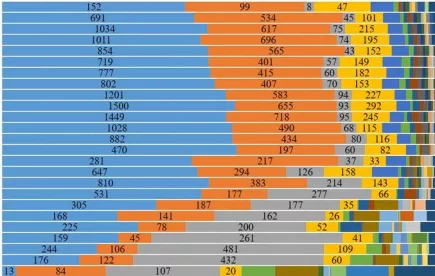
Deltacron recombinant XBC.1.6 at 30% of sequences in South Australia
We haven’t heard much about Deltacron recombinants recently, but one such variant is making real headway in South Australia – XBC.1.6 – is now at an astonishing 30% of SARS-CoV-2 sequences in that state. More...
Censored by TikTok: Gastroenterologist reveals damage to human microbiome by vaccines
“Their bifidobacteria dropped to like zero – from like a million to like zero – there was a persistence in the damage, not only 90 days but 6-9 months later. More...
China: 31 cases of XBB.1.9.1 – up from just two cases last week
China’s CDC has just published its latest report on Covid-19 variants circulating in the country, and XBB.1.9.1 has seen a significant increase in cases from last week when it recorded just 2 cases. More...
Covid-19 Origins: The Raccoon Dog’s Breakfast *5 Updates*
The recently published scientific report about raccoon dog DNA being found in the Wuhan wet market has created headlines around the globe, but almost no one has read it, and even fewer seem to be aware of its conclusions. More...