Shielding “would not have been a viable public health strategy for COVID-19”
Shielding the vulnerable while allowing infections to spread among the wider population would not have been a viable public health strategy for COVID-19 and is unlikely to be effective for future pandemics.
The COVID-19 pandemic, caused by the coronavirus SARS-CoV-2, has led to a wide range of non-pharmaceutical interventions being implemented around the world to curb transmission. However, the economic and social costs of some of these measures, especially lockdowns, has been high.
An alternative and widely discussed public health strategy for the COVID-19 pandemic would have been to ‘shield’ those most vulnerable to COVID-19 (minimising their contacts with others), while allowing infection to spread among lower risk individuals with the aim of reaching herd immunity. Here we retrospectively explore the effectiveness of this strategy using a stochastic SEIR framework, showing that even under the unrealistic assumption of perfect shielding, hospitals would have been rapidly overwhelmed with many avoidable deaths among lower risk individuals.
Crucially, even a small (20%) reduction in the effectiveness of shielding would have likely led to a large increase (>150%) in the number of deaths compared to perfect shielding. Our findings demonstrate that shielding the vulnerable while allowing infections to spread among the wider population would not have been a viable public health strategy for COVID-19 and is unlikely to be effective for future pandemics.
Peer reviewed study: Critical weaknesses in shielding strategies for COVID-19
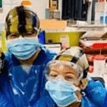
UK: Admission and Care of Residents during COVID-19 Incident in a Care Home
Image by Michael Bußmann from Pixabay