Tag: B.1.617
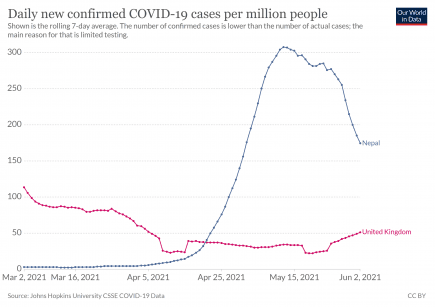
The “Nepal Variant” – does it exist or is it just racist fearmongering?
There’s plenty of coverage in the UK press today about a so-called “Nepal Variant” of Sars-CoV-2. More...
Preprint: B.1.617 coronavirus variants show enhanced spike cleavage by furin
“The spike (S) glycoprotein of the SARS-CoV-2 virus that emerged in 2019 contained a suboptimal furin cleavage site at the S1/S2 junction with the sequence 681 PRRAR/S 686. More...
Angola: Increase in coronavirus infections, hospitalisations and deaths as 2nd wave peaks
Lubango central hospital in Angola is under pressure due to the growing number of patients, reporting the possible collapse of the system. More...
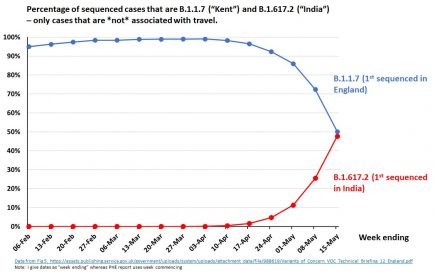
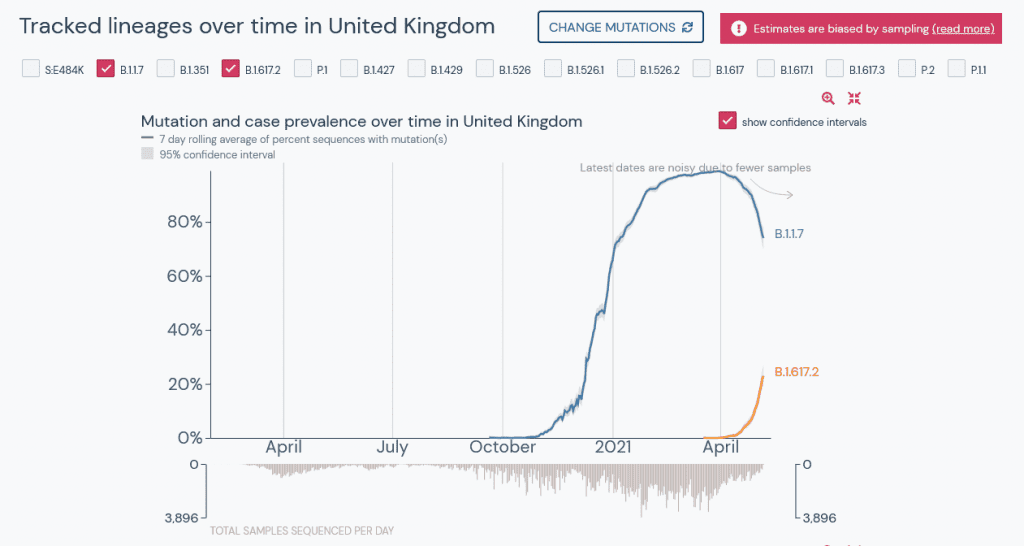
UK: PHE data shows B.1.617.2 now outcompetes B.1.1.7
More amazing work by Prof. Christina Pagel in deciphering the latest Public Health England data dumps for B16172. More...
France: 46 cases of B.1.1.7 with E484Q mutation in Bordeaux coronavirus outbreak of VOC 20I/484Q
The French city of Bordeaux is to fast-track vaccinations for residents in one neighbourhood, opening access the jab for all adults after nearly 50 people tested positive for a “very rare” variant of Covid-19.
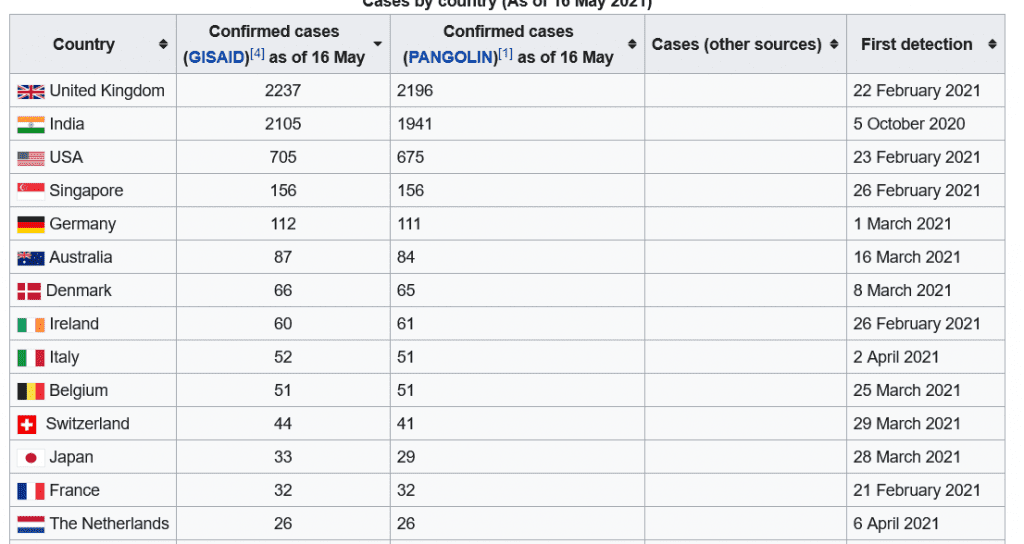
UK: more cases of Delta coronavirus variant found in Britain than in India
B.1.617 cases as of 16th May 2021 as per Wikipedia
And yes, we KNOW it’s because there is far more sequencing done in the UK than in India. More...
Singapore: Changi Airport coronavirus cluster – 18 patients with 61% vaccine breakthrough rate
Eleven out of 18 positive patients were vaccinated, at least 6 are infected with the B.1.617 variant. More...
UK: B.1.617.2 Delta coronavirus variant cases double in four days to 2,323
The number of confirmed UK cases of the Covid variant first detected in India has almost doubled in four days, Health Secretary Matt Hancock said, as experts warned it could become the dominant type of the virus imminently. More...
Canada CDC: ‘Researchers are monitoring for … B.1.617.4’
British Columbia CDC: “Researchers are monitoring for specific sublineages of this variant, including B.1.617.1, 1.617.2, B.1.617.3 and B.1.617.4” (is this a typo?) More...