Tag: VOC
Israel: arrival of Lambda variant would trigger a lockdown
The Israeli Health Ministry on Monday warned that new coronavirus variants from abroad could force Israel into a lockdown that the government is working hard to avoid, with the Lambda variant posing a particularly pressing threat. More...
UK: PHE Technical Briefing and Variants of Concern update 18
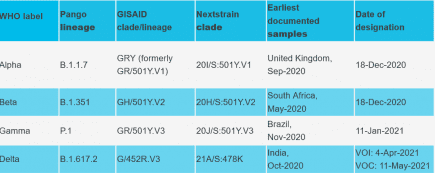
PHE England have recently published new reports on the SARS-COV-2 variants circulating in Britain: Alpha, Beta, Gamma, Zeta, Eta, B.1.1.318, Theta, Kappa, B.1.617.3, AV.1, C.36.3, Lambda, C.37
SARS-CoV-2 variants of concern and variants under investigation in England
Variants under surveillance
Variant prevalence
Secondary attack rates
SARS-CoV-2 Immunity and Reinfection Evaluation (the SIREN study) cohort monitoring
Part 2: Delta (B.1.617.2) surveillance
Surveillance through genomic data
Delta with K417N (Delta-AY.1)
Investigation of SARS-CoV-2 variants of concern: routine variant data update
Data on individual variants
Alpha
Beta
Gamma
International Epidemiology
Zeta
Eta
VUI-21FEB-04 (B.1.1.318)
Theta
Kappa
VUI-21APR-03 (B.1.617.3)
VUI-21MAY-01 (AV.1)
VUI-21MAY-02 (C.36.3)
Lambda (C.37, VUI-21JUN-01)
More...
UK: learning to live with COVID-19 cannot mean simply allowing infections to spread unchecked causing hospitalisations, illness – including Long COVID, and deaths
Joint Statement from the Association of Directors of Public Health and the Faculty of Public Health on the COVID-19 Roadmap. More...
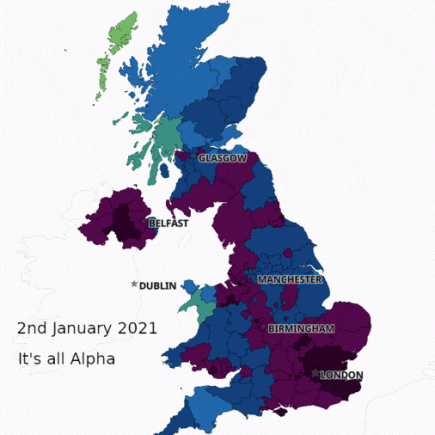
From Alpha to Delta – how Britain won and then lost the fight against coronavirus
After months of being ravaged by the Alpha variant (B.1.1.7) in 2020, Britain seemed to turn a corner in its fight with the coronavirus in early 2021. More...
Australia: “non-infectious chronic shedder” tests positive after discharge from coronavirus quarantine hotel
Australian health authorities are contacting scores of people in Western Australia after a man tested positive to COVID-19 after being released from the state’s quarantine hotels. More...
Vietnam: No new hybrid coronavirus strain detected in Vietnam says WHO
“There is no new hybrid variant in Vietnam at this moment based on WHO definition,” Kidong Park, the WHO representative in Vietnam, told Nikkei Asia on Wednesday. More...
WHO announce new names for Sars-CoV-2 coronavirus variants
The WHO have announced new names for the confusingly named sars-cov-2 variants. More...
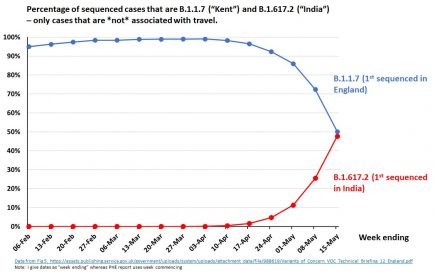
UK: PHE data shows B.1.617.2 now outcompetes B.1.1.7
More amazing work by Prof. Christina Pagel in deciphering the latest Public Health England data dumps for B16172. More...
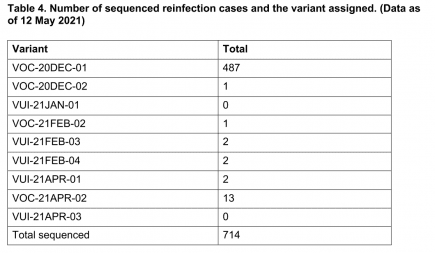
UK: 487 reinfections for UK coronavirus variant B.1.1.7 and 13 reinfections already for B.1.617.2
The latest UK PHE technical report shows that there have been 487 cases of reinfection recorded for the UK variant B.1.1.7. More...
Cameroon: travel-driven emergence and spread of SARS-CoV-2 lineage B.1.620 with multiple VOC-like mutations and deletions in Europe
“In this study we have presented evidence that a SARS-CoV-2 lineage designated B.1.620, first detected in Europe in late February, is associated with Central Africa, where it appears to circulate at very high prevalence, and has been introduced into Europe and the US on multiple occasions. More...